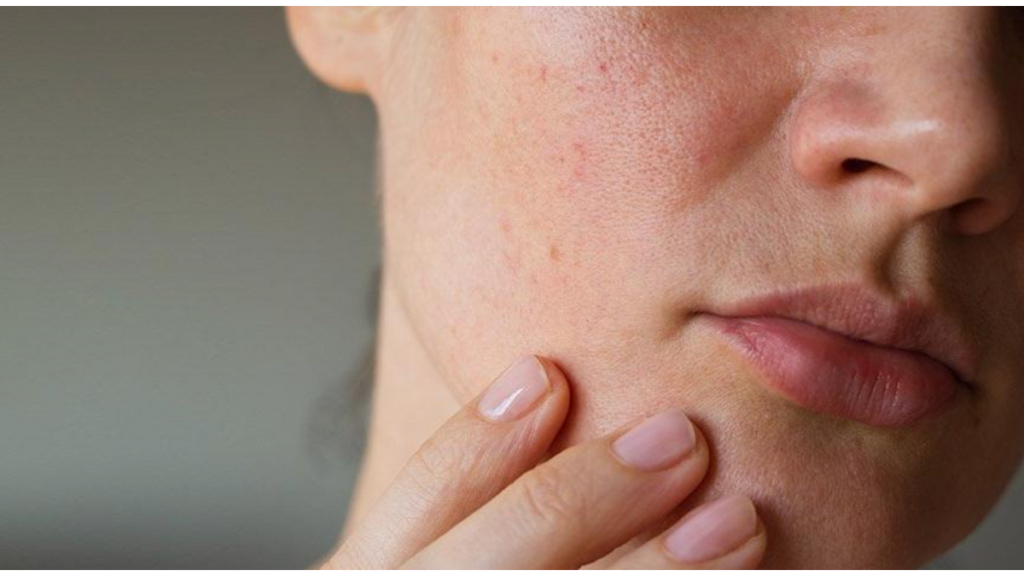
Milialar disease is an illness that affects the quality of life of its victims but is still relatively rare. In this post, we will discuss milialar disease, including its definition, possible causes, typical symptoms, and accessible treatments. Understanding this illness is vital for both patients and healthcare providers, as it can help in early identification and appropriate management.
What Is Milialar Disease?
Definition
Milialar disease, commonly known as Milia, is a skin ailment characterized by the development of tiny cysts or bumps that can be either white or yellow in color. These cysts, also known as milia, range in size from roughly 1 to 2 millimeters.
Types of Milia
- Primary Milia: Babies frequently have them, and they tend to appear on the cheeks and nose. In most cases, they go away on their own within a couple of weeks.
- Secondary Milia: These are secondary conditions, meaning they result from other skin issues or injuries, such as burns, blisters, or overexposure to the sun.
- Neonatal Milia: These are similar to primary milia in that they manifest in neonates but often disappear within a few weeks.
- Miliaen Plaque: Inflammation surrounds a cluster of milia in this form. It happens infrequently.
Causes of Milialar Disease
Keratin, a protein found in the skin’s outermost layer, becomes trapped under the epidermis and causes milia. It’s not always easy to pin down what exactly causes them, but these things are likely contributors:
- Skin Trauma: Secondary milia can be caused by skin injuries such as burns or blisters.
- Skin Care Products: Makeup that is too thick or oily can clog pores and encourage the growth of milia.
- Sun Exposure: Miliaria are more likely to appear after prolonged exposure to the sun’s UV rays.
- Genetics: Milia may have a genetic component that makes them more likely to appear in certain people.
Symptoms of Milialar Disease
Milial illness is characterized by the development of tiny bumps that can be either white or yellow in color. These cysts form in the face, cheeks, nose, and eyes and are typically painless. Possible further signs include:
- Inflammation and redness in the vicinity of the injury.
- Itchiness or pain, particularly if the cysts become inflamed.
- A bigger, lumpy patch of cysts is a possible symptom of miliaen plaque.
Diagnosis and Treatment
· Diagnosis
Miliaria are normally diagnosed by a dermatologist after a thorough skin examination. A biopsy may be necessary to rule out other skin disorders in some circumstances.
Treatment Options
- Topical Retinoids: There are several drugs that can be used to treat a variety of conditions.
- Laser Therapy: Milia can be eliminated with a laser treatment that vaporizes the cysts.
- Cryotherapy: The cysts are frozen using liquid nitrogen before being extracted.
- Chemical Peels: The cysts are exfoliated and removed from the skin by applying a chemical solution.
- Needle Extraction: The cysts can be easily pierced and extracted by a dermatologist using a sterile needle.
Prevention
Here are some things to keep in mind to avoid getting milia:
Choose skincare products that won’t clog your pores.
Don’t slather on the thick, oil-based makeup.
Wear sunscreen to prevent skin damage from the sun.
Conclusion
Milia is a cosmetically bothersome but otherwise innocuous skin disease. Effective symptom management is vital for people of all ages and all conditions. See a dermatologist for an examination and advice if you think you have milia or other skin problems.
Read More : rubblemagazine.com
FAQs (Frequently Asked Questions)
Are milia contagious?
No, milia are not contagious and cannot be spread from person to person.
Can I remove milia at home?
It is not recommended to try and remove milia at home, as improper extraction can lead to infection or scarring. Consult a dermatologist for safe removal.
Do milia go away on their own?
Primary milia in infants often disappear on their own, but other types may require medical intervention for removal.
Are there any dietary changes that can help prevent milia?
While a healthy diet is essential for overall skin health, there is no specific dietary change known to prevent milia.
Can milia be a sign of an underlying health condition?
Milia are typically a benign skin condition and are not indicative of underlying health issues. However, if you have concerns, it’s best to consult with a healthcare professional.